Winter 2025 (Volume 35, Number 4)
Survey Results:
Administrative Burden
Download PDF
In this issue’s Joint Count survey, the CRA External Relations Committee polled the CRA membership about how increasing administrative burden associated with completing insurance forms is affecting members, in order to better understand the scope and impact of this issue nationwide. The survey received 94 responses, the most responses to any Joint Count survey in recent years. Respondents represented a broad cross-section of Canadian rheumatologists.
The first part of the survey asked members “Are you regularly required to complete insurance forms for patients to access medication?” A striking 99% of respondents answered "yes".
When asked if this was an issue, almost 96% of respondents affirmed that this requirement poses a significant issue in their clinical workflow.
In response to the question “Do you typically have additional forms to complete after the initial application was submitted to insurance to start a new medication?”, 76% of respondents noted that additional forms are typically required after the initial insurance application, further compounding the administrative burden. The additional forms come from a variety of sources, including insurance providers (95.7%), third parties
(e.g. Benefit Plan Managers 61.4%), and other sources such as provincial special access programs, pharmaceutical companies and compassionate access pathways (12.9%).
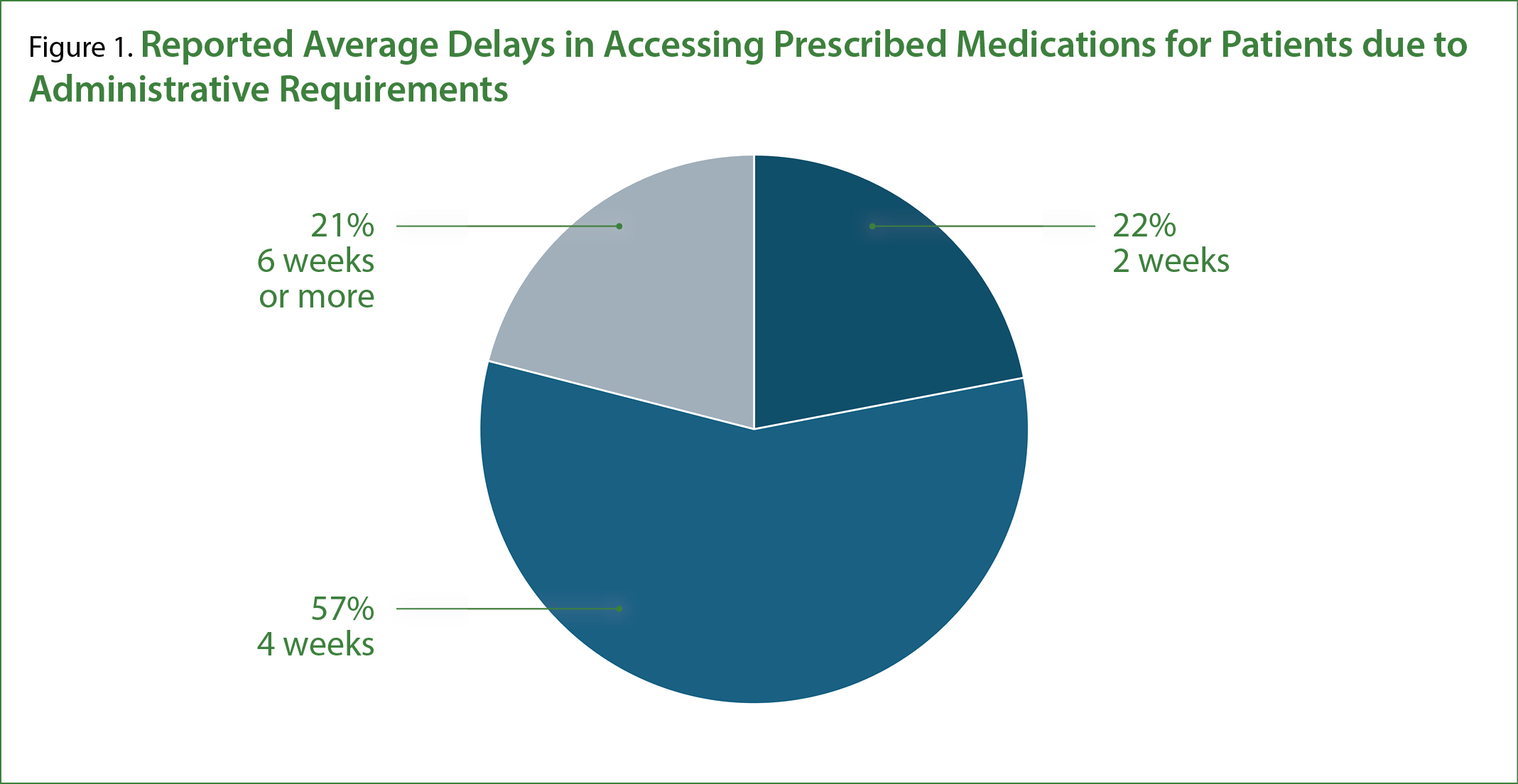
As shown in Figure 1 above, 78% of respondents reported experiencing unreasonable delays in accessing prescribed medications due to administrative requirements, with 57% reporting an average 4-week delay, 22% citing a 2-week delay, and 21% experiencing delays of 6 weeks or more.
Qualitative feedback from this survey highlighted the burnout and emotional toll from repetitive paperwork, the need for standardized forms, inconsistencies across insurance providers, and the impact on patient care, especially in urgent cases (e.g. tocilizumab for giant cell arteritis, off-label biologics for myositis or CNS vasculitis).
Overall, this survey underscores the significant administrative burden faced by Canadian rheumatologists in securing medication access for their patients. The CRA External Relations Committee will use these findings to advocate for streamlined processes, standardized forms, and improved communication pathways with insurers.
For questions or feedback, please contact info@rheum.ca.
|
-EN-v2.gif)

-EN-v2.gif)

