Winter 2022 (Volume 32, Number 4)
A Wandering Arthritis and Mind
By Bijalpen Patel, MD; and Jennifer Shiroky-Kochavi, MD, MPH
Download PDF
|
Case Presentation:
|
A 20-year-old university student, originally from Chicago, presented
to our primary care clinic for an emergency room (ER) visit follow-up.
His medical history was notable for pneumonia complicated by
acute respiratory distress syndrome 3 years prior. Over the previous
6 weeks, he had multiple urgent care visits for left hip, knee, and ankle
pain and swelling associated with fevers and chills. These symptoms
were preceded by abdominal discomfort, nausea, vomiting,
and rectal pain that he assumed was due to a hemorrhoid. Generalized
arthralgias and myalgias had more recently developed in addition
to his left lower extremity articular pain and swelling. Within this
time period, he experienced an unintentional 40-pound weight loss.
The morning of the emergency room visit he had consulted with an orthopedic
surgeon who recommended an autoimmune workup. Later
that day, the patient presented to the ER due to intolerable pain with
his chief complaint documented as “I have an undiagnosed autoimmune
disease.” During the visit, he was found to have a 2.9 cm left perianal abscess
on computed tomography (CT) scans of the abdomen and pelvis. The abscess
was incised and drained, and he was discharged with a recommendation for sitz
baths and non-steroidal anti-inflammatory drugs (NSAIDs) as needed for pain relief.
He was not prescribed antibiotics. Unfortunately, wound cultures were not sent.
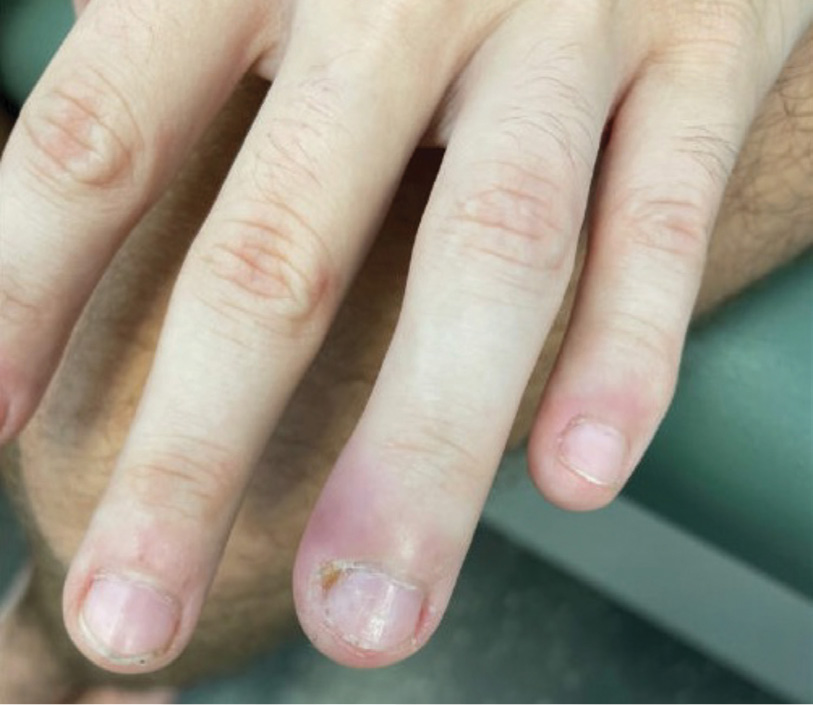
At the time of presentation to our clinic, his exam was notable for tachycardia, hypotension,
painful oropharyngeal ulcers, cervical lymphadenopathy, swelling along
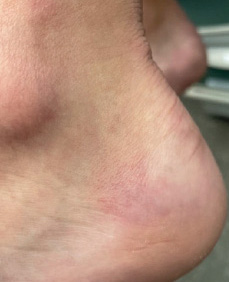
multiple nail folds, mild tenderness and swelling of the left knee and ankle, and tender
nodules on both heels (Figures 1 and 2). We directly admitted him to the hospital
for expedited infectious and autoimmune workup. Infectious workup, including urine
and serum sexually transmitted infection studies and extensive stool studies, were all
negative. Anti-nuclear antibodies (ANA) were negative, rheumatoid factor (RF) and
anti-cyclic citrullinated peptide (anti-CCP) undetectable, and HLA-B27 screen was
negative. CT chest visualized subtle subcentimeter ground-glass opacities. Magnetic
resonance imaging (MRI) of the lumbar spine and pelvis was negative for axial
inflammatory changes. Inpatient endoscopy and colonoscopy did not visualize any
findings to suggest inflammatory bowel disease. He was discharged with a suspected diagnosis of reactive arthritis (ReA)
presumptively triggered by gastroenteritis and the perianal abscess. Fevers and migratory arthritis resolved over the following
4 weeks with daily ibuprofen.
|
|
Figure 1.
|
|
|
Figure 2.
|
Following this hospitalization, he developed new daily anxiety and a sense of hopelessness in the setting of a prolonged
acute illness without definitive diagnosis and his complicated hospitalization. He described the multiple procedures
during his hospitalization as traumatizing. He reported having difficulty sleeping with frequent awakenings from nightmares
about the hospitalization and fears surrounding his illness. Mood symptoms improved in the following months
with initiation of a selective serotonin reuptake inhibitor (SSRI) and consulting with a psychologist for Cognitive Behavioral
Therapy.
His diffuse arthralgias recurred 1 month after resolution, with once again an elevated erythrocyte sedimentation rate
(ESR) of 49, but undetectable C-reactive protein (CRP). His symptoms again improved with ibuprofen. His working diagnosis
transitioned to chronic non-radiographic axial and peripheral spondyloarthritis, currently being managed with
meloxicam as needed. Imaging studies continued to be negative for inflammatory changes. |
Introduction
Reactive arthritis (ReA) is a subset of spondyloarthritis defined
as inflammatory arthritis triggered by a gastrointestinal
or genitourinary tract infection.1,2 Due to the absence of
agreed-upon clinical criteria, specific diagnostic findings, and
variable disease course, ReA remains a challenging diagnosis
to make, requiring a clinician well-versed in rheumatology.
Epidemiology
ReA typically affects young adults between the ages of
18 and 40 years with no difference in incidence among
males and females with gastrointestinal triggers, and increased
incidence in males with preceding genitourinary
infection. White individuals appear to be at increased risk
of developing ReA, which is attributed to the higher frequency
of the HLA-B27 gene in this demographic.3,4 Gastrointestinal
infections due to Shigella, Campylobacter,
and Yersinia have about a 1-1.5% incidence of leading to
ReA, while genitourinary infections, such as Chlamydia
trachomatis have a 4-8% incidence.5
Clinical Features
Rheumatic symptoms often present 1-4 weeks after the
infection has resolved, which can make it challenging to
identify an association.2,4 ReA most commonly presents
as an acute asymmetric oligoarthritis that can involve
both small and large joints, as well as the axial skeleton.
Joint involvement can exhibit an additive or migratory
course. Extra-articular musculoskeletal manifestations
include enthesitis, bursitis, and dactylitis.1,2,4
Mucosal and ocular involvement are common. Ocular
symptoms typically present as uveitis or conjunctivitis. Mouth
ulcers are typically painless. Rashes unique to ReA include
keratoderma blennorhagicum, a pustular lesion commonly
seen on the plantar surfaces, and circinate balanitis, painless
psoriasiform lesions over the glans or shaft of the penis.1,2,4
Cardiac symptoms are uncommon and include conduction
abnormalities, aortic regurgitation, and pericarditis.1
Diagnosis
No diagnostic criteria have been established for ReA. The
American College of Rheumatology last issued general
guidelines in 1999, which were restricted to symptoms following
an enteritis, urethritis and cervicitis with positive
cultures for Chlamydia or enterobacteria, or persistent synovial
infection.2,4,6 In practice, the diagnosis is made based
on the totality of the clinical picture, with increased likelihood
in the setting of positive infectious work-up.7 Given
the non-specific arthritic pattern, work-up often includes investigating
multiple autoimmune and infectious etiologies,
with ReA ultimately being a diagnosis of exclusion.
ReA may be a self-limiting disease but it does not
always fully resolve. About 65% of patients progress into
the chronic arthropathy category with persistent symptoms
for greater than 6 months.2,3 Therefore, it is important
to recognize the disease early and provide appropriate
counselling and treatment for patients.
ReA should be suspected in individuals with sudden onset
inflammatory arthropathies following a recent infection.
However, a prodromal infection cannot always be identified;
asymptomatic or minorly symptomatic infections can trigger
ReA. A thorough history should include any preceding infections
and a sexual history. There are no pathognomonic
lab results or imaging findings for ReA. ESR and CRP will be
elevated in the acute phase, and trend down in the chronic
stage of the disease. Radiographs may visualize joint space
narrowing, swelling, erosions, or bony spurs.2,7
Approximately 50-80% of patients with ReA also test
positive for the HLA-B27 gene. The presence of HLA-B27
has been associated with an increased risk of severe symptoms
and progression to chronic disease.2-4,6 HLA-B27 genes
contribute to the persistence of bacteria within the body,
which is suspected to be the reason behind the high risk of
developing severe ReA in these patients.3
Therapeutic Approach
The goals of treatment focus on decreasing pain and inflammation,
minimizing disability and monitoring for
relapse or progression to chronic disease.
Patients are initially managed with NSAIDs until the
episode resolves. In situations where NSAIDs are contraindicated,
such as renal impairment, a history of gastrointestinal
disease, or significant cardiovascular disease, intra-articular
glucocorticoid injections are preferred. When ReA
has progressed and the disease involves multiple joints,
patients may benefit from systemic glucocorticoids. In this
case, it is important to provide peptic ulcer disease prophylaxis
and assess risks for osteoporosis as well.2
Although ReA is most likely to occur following an
infection, antibiotics are only indicated if evidence of
missed, untreated or persistent infection is found.
When symptoms are uncontrolled despite initial therapy
or if they last longer than 6 months, it is reasonable
to introduce disease-modifying antirheumatic drugs
(DMARDs). Sulfasalazine and methotrexate are most often
the preferred agents. In severe cases of ReA where there
is no improvement after 12 weeks of DMARD therapy, patients
may be candidates for initiation of biologic therapy
with anti-tumor necrosis factor agents.2,5 In several studies
looking at patients’ responses to biologic therapy, it is important
to note that patients had significant improvements
in their symptoms without major side effects reported.3
Adjusting to Uncertainty and Chronic Illness
Fears surrounding what an autoimmune disease could
mean prompted our patient’s emergency room visit. Following
his subsequent hospitalization, our patient struggled
with disabling anxious and demoralizing thoughts following
his clinical presentation, ultimately leading him to
take a short-term break from university and return home.
He had requested a leave of absence, which was unfortunately
denied by his academic institution. Like many rheumatologic
conditions, including ReA, adjustment disorders
(AD) are a slippery and difficult diagnosis to make.
All individuals experience and respond to stressful
events throughout their lifetimes, including issues with
their health. AD refers to maladaptive emotional or behavioural
responses to a stressor that lead to excessive
distress and daily functional impairment. The responses
are either discordant from the socially or culturally expected
reactions and/or cause marked distress or impaired
functioning.5 It fills a unique space along the spectrum of
psychological conditions as a transitional, subsyndromal,
or subclinical disorder. Similar to ReA, either the disorder
resolves or it persists and after a certain time meets criteria
for a more well-defined mental health condition.8-11
The similarities between ReA and AD do not stop with
their tempo. Both respective clinical specialties have long
worked with vague and understudied understandings of
these conditions. In the past decade the mental health community
has increasingly acknowledged the lack of research
on AD and pushed to better define the disorders. Both the
Diagnostic and Statistical Manual of Mental Disorders-5th
edition (DSM-5) and the International Statistical Classification
of Diseases and Related Health Problems, 11th edition
(ICD-11) have recently provided clearer frameworks
for this historically vague condition.8-11
Like ReA, AD requires an astute and experienced clinician
within the field to make a diagnosis. However, specialized
training is not required to assess and address psychological
struggles within our patients. Mental health disorders
are common among individuals with chronic inflammatory
disease and carry significant morbidity.12-14 Providers who
care for individuals with chronic inflammatory conditions
should feel comfortable screening for mood disorders, prescribing
common treatments, and connecting patients with
psychiatry and psychotherapy, treating disorders in tandem.
Conclusion
ReA, as well as adjustment disorders, largely remains a
clinical diagnosis relying on clinical acumen. Both conditions
provide poetic examples of what it means to practice
medicine. To practice the art of medicine is the privilege
to journey alongside a patient. We cannot always prevent,
predict, or cure, but we can make the journey easier. We
can acknowledge the psychological and emotional impacts
on those living with the diagnoses we make, the
uncertainty we navigate and the guidance we provide. In
caring for this patient, we were unable to predict his disease
course with certainty. However, it was critical to simultaneously
acknowledge the psychological and social
impact of his symptoms, along with addressing the physical
distress in order to care for him appropriately.
|
Back to the Case
|
Preparing this review allowed the opportunity to revisit
how we might have approached this case differently if
we were given another chance. Knowing what we know
now, it would have been helpful to have had results from
urethral and rectal swabs to assess for Chlamydia trachomatis
further, and wound cultures from the perianal abscess.
Results from knee or ankle arthrocentesis would
have also helped solidify a diagnosis.
Like many stories of the presentation and progression of
autoimmune conditions, our case does not comfortably
fit within the illness script for ReA. While ReA progressing
to chronic non-radiographic axial and peripheral
spondylarthritis remains the working diagnosis, the patient
continues to lack definitive findings. The patient
was lost to follow-up for 6 months due to improvement
in symptoms. He returned to university without issue.
While preparing this manuscript, he reconnected with
us due to recurrence of fatigue and arthralgias similar to
his presentation last year, and a new erythematous rash
around his neck and upper chest. He reported that, in the
interim, the only symptom that did not resolve was very
difficult to treat acne, primarily on his face and scalp, but
also appearing along his chest, back and extremities. He
reports ancestry from Italy and Ireland. He is currently
undergoing workup for other uncommon autoinflammatory
diseases, including Behçet Disease, Familial Mediterranean
Fever, and Adult-onset Still’s Disease.
|
Bijalpen Patel, MD
Internal Medicine Resident
University of South Florida Morsani College of Medicine
Tampa, Florida
Jennifer Shiroky-Kochavi, MD, MPH
Assistant Professor, General Internal Medicine
University of South Florida Morsani College of Medicine
Tampa, Florida
References:
1. Garcia-Kutzbach A, Chacon-Suchite J, Garcia-Ferrer H, et al. Reactive arthritis: update 2018. Clin Rheumatol.
2018;37(4):869-874.
2. Jubber A. & Moorthy A. Reactive arthritis: a clinical review. J R Coll Physicians Edinb. 2021;51(3): 288-297.
3. Zeng H, Luo B, Zhang Y, et al. Treatment of reactive arthritis with biological agents: a review. Biosci Rep.
2020; 40(2).
4. Selmi C. & Gershwin ME. Diagnosis and classification of reactive arthritis. Autoimmun Rev. 2014; 13: 546-9.
5. Wendling D, Prati C, Chouk M, et al. Reactive arthritis: treatment challenges and future perspectives. Curr
Rheumatol Rep. 2020; 22(7):29.
6. Sieper J, Braun J, Kingsley GH. Report on the fourth international workshop on reactive arthritis. Arthritis
Rheum. 2000:43;720-34.
7. Sieper J, Rudwaleit M, Braun J, et al. Diagnosing Reactive Arthritis. Arthritis Rheum. 2002;46: 319-27.
8. American Psychiatric Association. Trauma- and stressor-related disorders. In Diagnostic and Statistical Manual
of Mental Disorders, 5th ed.; American Psychiatric Association Publishing: Washington DC, USA, 2013.
9. World Health Organization. World Health Organization International Statistical Classification of Diseases
and Related Health Problems, 11th ed.; World Health Organization: Geneva, Switzerland, 2019.
10. O’Donnell ML, Agathos JA, Metcalf O, et al. Adjustment disorder: current developments and future directions.
Int J Environ Res Public Health. 2019;16:2537.
11. Bachem R, Casey P. Adjustment disorder: A diagnosis whose time has come. J Affect Disord. 2018;
227:243-53.
12. Benros ME, Waltoft BL, Nordentoft M et al. Autoimmune disease and severe infections as a risk factor for
mood disorders: a nationwide study. JAMA Psychiatry. 2013;70(8):812-20.
13. Moussavi S, Chatterji S, Verdes E, et al. Depression, chronic diseases, and decrements in health: Results
from the World Health Surveys. Lancet. 2007;370:851-858.
14. He Y, Zhang M, Lin EHB, et al. Mental disorders among persons with arthritis: Results from the World
Mental Health surveys. Psychological Medicine. 2008;38(11):1639-50.
|
