Winter 2014 (Volume 24, Number 4)
Make the First Break the Last! Fracture Liaison Services (FLS)
By Diane Theriault, MD, FRCPC, CCD
Download PDF
The Problem
After they break a bone, fewer than 20% of fragility fracture patients ever receive the bone mineral density (BMD) evaluation and/or treatment they require for their underlying osteoporosis. Countless Canadians go on to suffer debilitating repeat fractures because of this huge care gap.
Fractures are Common
One in three women and one in five men will suffer a fracture during their lifetime. The overwhelming majority of these fractures are due to osteoporosis (Figure 1).
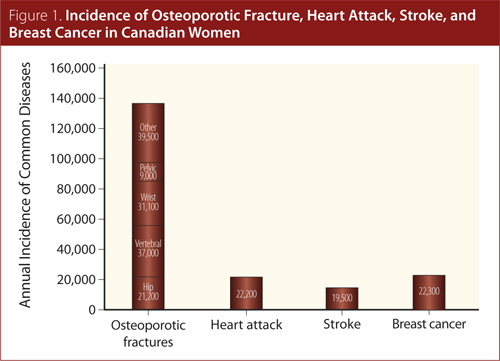
Fractures Beget Fractures
• 14% of wrist fracture patients will suffer another fracture within three years.
• 20% of vertebral fracture patients will suffer another vertebral fracture within one year.
• 9% of hip fracture patients will break the other hip within one year.
• Of patients with hip fractures, half have “warned” physicians in advance that they were at high risk when they suffered a prior “signal” fracture.
• Many secondary fractures can be avoided with effective drug treatment.
The Cost-effective Solution: FLS
FLS is a systematic approach that ensures that all patients who present with a “signal” fracture receive the osteoporosis care they need to prevent future fragility fractures. Support for FLS is growing around the world, and while Canada is seen as an innovative leader, there is a long way to go. Most Canadian hospitals do not have an FLS—indeed, most provinces do not have any FLS!
How Does it Work?
A dedicated FLS coordinator (usually a nurse or nurse practitioner) intervenes immediately after a first fragility fracture to ensure that all fracture patients have a comprehensive fracture risk-assessment, and then receive treatment as warranted to prevent the next fracture. The steps in the process are:
• Identification: all men and women over 50 years of age who present with fragility fractures will be assessed for risk factors for osteoporosis and future fractures.
• Investigation: as per the 2010 Osteoporosis Canada Guidelines, those at risk will undergo BMD testing.
• Initiation: where appropriate, osteoporosis treatment will be initiated.
Under this “3-i” model, the dedicated FLS staff coordinate the patient’s care, working within the protocols of the institution and under the direction of a physician with expertise in osteoporosis.
What Does Success Look Like?
The FLS model of care has been shown within Canada and many other countries to eliminate the post-fracture osteoporosis care gap, reducing the incidence of repeat fractures, reducing mortality, and resulting in significant cost savings. When formal cost‐effectiveness analyses are done, even when considering all costs (including additional BMD tests performed and additional osteoporosis medications prescribed), the 3-i FLS model is consistently proven to be the most cost effective.
What You Can Do To Help
Rheumatologists can become engaged and respected as local champions for FLS. Implementing an FLS from scratch is not an easy task. For this reason, Osteoporosis Canada has developed an FLS Toolkit to facilitate matters. This Toolkit contains comprehensive background information on FLS including province-specific information and templates for various documents (algorithms, job descriptions, form letters to primary care providers, etc.) which can be downloaded and adapted to fit the needs of individual institutions.
Make the First Break the Last! by joining the campaign to improve osteoporosis care for fragility fracture patients in your community. More information, resources, and practical guidance on the implementation of FLS can be found at www.osteoporosis.ca/fracture-liaison-service. Join Osteoporosis Canada’s FLS Network (for free!) and you will receive regular updates and invitations to webinars on topics related to FLS and post-fracture care. You can also contact me at dtheriault@osteoporosis.ca.
Diane Theriault, MD, FRCPC, CCD
Rheumatologist
Chief Scientific Officer,
Fracture Liaison Services,
Osteoporosis Canada
Dartmouth, Nova Scotia |



